Bariatric Center
Let’s build a lighter, brighter future together
Weight loss surgery in New Jersey
At Mountainside Medical Center, we understand that weight loss surgery is a big decision that can change your life. That’s why our bariatric doctors are prepared to answer your questions and offer you support every step of the way on your weight loss journey. We offer weight loss seminars and a variety of surgical treatments, including gastric bypass and sleeve gastrectomy, for patients who are eligible for bariatric surgery. Whenever possible, we also offer minimally invasive techniques and laparoscopic surgery to help reduce scarring and speed up recovery times.
To learn more about our weight loss surgery treatments, please call
(973) 429-6500Preoperative weight loss evaluations
When diet, exercise and medication aren’t working, weight loss surgery may be an option for treating obesity. Research from The American Society for Metabolic & Bariatric Surgery shows that patients may lose as much as 60% of excess weight six months after weight loss surgery, and up to 77% of excess weight a year after surgery. The majority of patients also see comorbidities like diabetes, dyslipidemia, hypertension, and sleep apnea decrease or go away altogether after weight loss surgery.
You may be eligible for weight loss surgery if your body mass index (BMI) is higher than 40. If you have serious health conditions like diabetes or heart disease, bariatric surgery may be beneficial if your BMI is between 35 and 40. Patients with a BMI below 35 do not qualify for weight loss surgery.
If you’d like to learn more about bariatric surgery, attending a free seminar is a great place to start. Click here to browse our seminars.
Weight loss surgeries we offer
There are two types of weight loss surgery: restrictive procedures and malabsorptive procedures. Restrictive procedures aim to decrease your food intake by reducing the size of the stomach. Malabsorptive procedures bypass a portion of the food directly to the small intestines, limiting the amount of nutrients the body absorbs.
At Mountainside Medical Center, our skilled surgeons are trained to perform various bariatric surgical procedures. Whenever possible, your doctor will perform surgeries laparoscopically or using minimally-invasive techniques.
We offer the following weight loss surgeries:
- Gastric band (LAP Band) — During this restrictive procedure, a silicone band is placed around the top of the stomach. This creates a small pouch and a narrow passageway into the rest of the stomach, which limits the amount of food you can consume. The band is then inflated with a saline solution. When food enters the pouch, it slowly empties into the rest of your stomach. Liquid passes through the narrow passageway and denser foods are delayed from passing through. Adjustments to the gastric band occur six to eight weeks after your surgery, and as needed thereafter. This procedure is fully reversible.
- Roux-en-Y gastric bypass — This combined restrictive and malabsorptive procedure is the current gold standard procedure for weight loss surgery. During this procedure, the surgeon will separate the upper and lower portions of the stomach to create a small pouch. This pouch restricts the amount of food you can consume, which helps you feel full from smaller portions.
- Sleeve gastrectomy – During this restrictive procedure, the left side of the stomach is removed, leaving it smaller and roughly the size and shape of a banana. The nerves to the stomach and the outlet valve remain intact to preserve the function of the stomach while greatly reducing its volume.
After your surgery, our bariatric doctors will connect you with various resources, including support groups, dieticians, and other forms of follow-up care, to ensure you achieve your long-term weight loss goals.
If you’re ready to schedule a consultation
Call (973) 429-6500 or visit MountainsideHosp.com/find-physicianInsurance coverage for weight loss surgery
If you are considering bariatric surgery, you will need to call your insurance company to verify your plan includes bariatric benefits for the treatment of morbid obesity.
You will need the following information from your insurance company:
- Does your plan cover bariatric services and surgery, or is it an exclusion or only covered if life-threatening (meaning they do not cover bariatric surgery)?
- If your plan covers bariatric services and surgery, you will need to know what pre-surgical requirements are necessary to qualify for surgery. For example, Medicaid requires six consecutive months of medical weight management and psychological evaluation.
- What is your portion of the cost? Confirm how much your insurance will cover for the procedure.
In case you need to contact your insurance company again, write down the name of the representative you spoke to, as well as a reference number for the call.
Here are the specific codes your insurance company may request:
- ICD code of obesity E66.01
- CPT code for sleeve 43775
- CPT code for bypass 43644
Weightloss Surgery Options
Our Medical Director, Dr. Karl Strom, Explains Your Bariatric Surgery Options
According to the American Society for Metabolic and Bariatric Surgery, there are two basic approaches to weight loss surgery:
- Restrictive procedures that decrease food intake
- Malabsorptive procedures that alter digestion, causing food to be poorly digested and incompletely absorbed
Laparoscopic or Minimally Invasive Surgery Alternatives
At Hackensack Meridian Mountainside Medical Center, we perform the following minimally invasive surgeries:
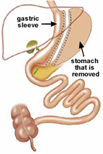
Sleeve Gastrectomy
Sleeve Gastrectomy
A Restrictive Procedure
The sleeve gastrectomy is an operation in which the left side of the stomach is surgically removed, leaving it roughly the size and shape of a banana. The nerves to the stomach and the outlet valve remain intact to preserve the functions of the stomach while drastically reducing its volume.
By comparison, when a gastric bypass (Roux-en-Y) procedure is performed, the stomach is divided rather than removed and it can be reconnected (reversed) if necessary. There is no intestinal bypass with sleeve gastrectomy procedures, only stomach reduction.
Advantages
- Sleeve gastrectomy involves no malabsorption of nutrients, therefore avoiding anemia, osteoporosis, protein deficiency and vitamin deficiency
- This is the only surgery that substantially removes the "hunger hormone," ghrelin.
- No adjustments or fills are needed.
- The chances of an ulcer occurring are minimized.
Risks
- This procedure involves stomach stapling. Therefore, leaks and other complications related to stapling may occur.
- Because the stomach is removed, it is not reversible. It can be converted to almost any other weight loss procedure.
- The smaller, remaining portion of the stomach may stretch.
- Foods that you eat now may cause discomfort, nausea or vomiting after your surgery.
- Gastric surgery puts you at higher than normal risk of developing gallstones and gallbladder disease.
Gastric Band (LAP BAND™)
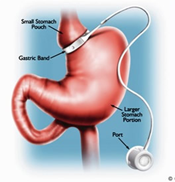
Gastric Band (LAP BAND™)
A Restrictive Procedure
The Laparoscopic Adjustable Gastric Banding procedure controls the amount of food that you can eat at one time. A hollow silicone band, placed around the top of your stomach, creates a small pouch and narrow passageway into the rest of the stomach, thereby limiting the amount of food you can consume. The band is then inflated with a saline solution. After food enters the pouch, it slowly empties into the rest of the stomach. Liquids pass through the narrow opening created by the band while denser foods are delayed from passing through.
Band adjustments occur six to eight weeks after surgery and as needed thereafter. For example, the band can be adjusted during pregnancy to allow for appropriate nutritional intake. Patients considering this procedure are carefully screened for dietary habits and preferences as well as pre-existing gastroesophageal reflux disease.
Advantages
- Gastric banding is the least invasive surgical option available and does not involve intestinal re-routing, cutting or stapling of the stomach wall or bowel.
- After LAP-BAND® Adjustible Gastric Band or other gastric banding procedures, patients can expect gradual weight loss for up to two years.
- This procedure is associated with reduced patient pain, length of hospital stay and recovery period.
- Adjustments may be performed without additional surgery, including during pregnancy.
- This is a fully reversible procedure.
Risks
- Band slippage or leakage may occur and can require an operation to correct the problem.
- Weight reduction after stomach banding surgery is typically slower than that following gastric bypass.
- Because a foreign body is implanted in the body, there is a risk of infection at the port-site.
- The band may erode into the stomach wall.
Gastric Bypass (Roux-en-Y)
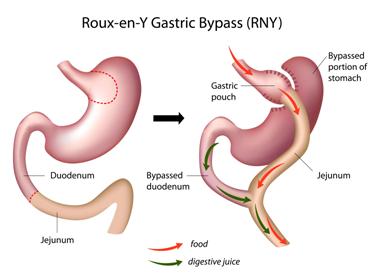
Gastric Bypass (Roux-en-Y)
A Combined Restrictive & Malabsorptive Procedure
In recent years, better clinical understanding of procedures combining restrictive and malabsorptive approaches has increased the choices of effective weight loss surgery for thousands of patients. By adding a technique called malabsorption, food is delayed in mixing with bile and pancreatic juices that aid in the absorption of nutrients. The result is an early sense of fullness, combined with a sense of satisfaction that reduces the desire to eat.
According to the American Society for Bariatric Surgery and the National Institutes of Health, Roux-en-Y gastric bypass is the current gold standard procedure for weight loss surgery. It is one of the most frequently performed weight loss procedures in the United States. In this procedure, stapling creates a small (15 to 20 cc) stomach pouch. The remainder of the stomach is not removed, but is completely stapled shut and divided from the stomach pouch. The outlet from this newly formed pouch empties directly into the lower portion of the jejunum, thus bypassing calorie absorption. This is done by dividing the small intestine just beyond the duodenum for the purpose of bringing it up and constructing a connection with the newly formed stomach pouch. The other end is connected into the side of the Roux limb of the intestine creating the "Y" shape that gives the technique its name. The length of either segment of the intestine can be increased to produce lower or higher levels of malabsorption.
Advantages
- The average excess weight loss after the Roux-en-Y procedure is generally higher in a compliant patient than with purely restrictive procedures.
- One year after surgery, weight loss can average 77% of excess body weight.
- Studies show that after 10 to 14 years, 50-60% of excess body weight loss has been maintained by some patients.
- A 2000 study of 500 patients showed that 96% of certain associated health conditions studied (back pain, sleep apnea, high blood pressure, diabetes and depression) were improved or resolved.
Risks
- Because the duodenum is bypassed, poor absorption of iron and calcium can result in the lowering of total body iron and a predisposition to iron deficiency anemia. This is a particular concern for patients who experience chronic blood loss during excessive menstrual flow or bleeding hemorrhoids. Women, already at risk for osteoporosis that can occur after menopause, should be aware of the potential for heightened bone calcium loss.
- Bypassing the duodenum has caused metabolic bone disease in some patients, resulting in bone pain, loss of height, humped back and fractures of the ribs and hip bones. All of the deficiencies mentioned above, however, can be managed through proper diet and vitamin supplements.
- A chronic anemia due to Vitamin B12 deficiency may occur. The problem can usually be managed with Vitamin B12 pills or injections.
- A condition known as "dumping syndrome" can occur as the result of rapid emptying of stomach contents into the small intestine. This is sometimes triggered when too much sugar or large amounts of food are consumed. While generally not considered to be a serious risk to your health, the results can be extremely unpleasant and can include nausea, weakness, sweating, faintness and, on occasion, diarrhea after eating. Some patients are unable to eat any form of sweets after surgery.
- In some cases, the effectiveness of the procedure may be reduced if the stomach pouch is stretched and/or if it is initially left larger than 15-30 cc.
- The bypassed portion of the stomach, duodenum and segments of the small intestine cannot be easily visualized using X-ray or endoscopy if problems such as ulcers, bleeding or malignancy should occur.
These procedures are known as laparoscopic. When a laparoscopic operation is performed, a tiny video camera and surgical instruments are inserted through small incisions made in the abdominal wall and the surgeon views the procedure on a separate high definition video monitor.
This provides the laparoscopic surgeon with better visualization and access to key anatomical structures while also eliminating the need for one long abdominal incision.
Studies have proven that patients who have laparoscopic weight loss surgery experience less pain after surgery, as well as easier breathing, improved lung function and higher oxygen levels. Other benefits of laparoscopy include fewer wound complications such as infection or hernia and a quicker return to pre-surgery activity levels.
Laparoscopic procedures for weight loss employ the same principles as their "open" surgery counterparts and produce similar excess weight loss. However, not all patients are candidates for this approach and all bariatric surgeons are not trained in the advanced techniques required to perform this less invasive method. The American Society for Bariatric Surgery recommends that laparoscopic weight loss surgery should only be performed by surgeons who are experienced in both laparoscopic and open bariatric procedures.
Weight loss surgery is major surgery. Although most patients enjoy an improvement in obesity-related health conditions (such as mobility, self-image and self-esteem) after the successful results of weight loss surgery, these results should not be the overriding motivation for having the procedure. The goal is to live better, healthier and longer. This surgery is only a tool. Your ultimate success depends on strict adherence to the recommended dietary, exercise and lifestyle changes.
A Lifelong Commitment
It is important to remember that there are no ironclad guarantees in any kind of medicine or surgery. There can be unexpected outcomes in even the simplest procedures. What can be said, however, is that weight loss surgery will only succeed when the patient makes a lifelong commitment? Some of the challenges facing a person after weight loss surgery can be unexpected. Lifestyle changes can strain relationships within families and between married couples. To help patients achieve their goals and deal with the changes surgery and weight loss can bring, most bariatric surgeons offer follow-up care that includes support groups, dieticians and other forms of continuing education.
Learn more by attending a free seminar
We’re here to help you start your journey to better health. We offer free seminars to explain every step of the weight loss process and what you can expect.
If you’re ready to schedule a consultation, call 973-429-6500 or visit mountainsidehosp.com/find-physician
Learn more about the success shared by others
You are not alone. Take a minute to read success stories from others that have already undergone bariatric surgery.




